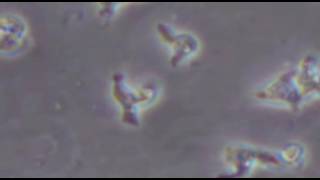
Deadly Parasitic Disease Finding Its Way to US Soil
Once thought to only be an issue for certain areas outside of the United States, cases of Leishmaniasis are on the rise as US soldiers deployed in Iraq and Afghanistan and ecotourists in South and Central America make their way home. New guidelines released by the Infectious Disease Society of America (IDSA) and the American Society of Tropical Medicine and Hygiene (ASTMH) this week highlight rapid diagnostic tests and innovative treatment strategies against this growing issue. The Centers for Disease Control and Prevention (CDC) lists Leishmaniasis as a term used to classify multiple clinical syndromes caused by an infection with Leishmania parasites. The disease is most commonly spread by the bite of an infected sand fly, an insect about one-third the size of a mosquito. According to the CDC, the disease primarily impacts individuals located in “the tropics, subtropics, and southern Europe.” Recent research has uncovered that US travelers and soldiers have started presenting with the infection—causing great concern for US doctors—spurning the development of these guidelines, “the first in the United States.” Because Leishmaniasis is a relatively unheard of infection in the United States, many of the doctors who are encountering these patients do not even consider it when diagnosing patients’ symptoms. Complicating matters further is the fact that, “the sore at the site of the infected sand fly bite is often painless, and symptoms of the infection may not show up for a month or longer,” according to the press release. Over 20 different types of Leishmania parasites exist and each one contributes to a different clinical syndrome of the disease. The most common form of Leishmaniasis is cutaneous leishmaniasis, known to cause sores on the skin which evolve into ulcers. The second most common form is visceral leishmaniasis. This life-threatening form of the infection affects the internal organs, such as the “spleen, liver, and bone marrow,” causing swelling of the spleen and liver, as well as fever, weight loss, and low blood counts. The third most common form is mucosal leishmaniasis. This form is thought to be “a sequela (consequence) of infection with some of the species (types) of the parasite that cause cutaneous leishmaniasis in parts of Latin America.” Mucosal leishmaniasis impacts the mucous membranes—particularly the mouth and nose—and can cause scarring if left untreated. The guidelines advise doctors that encounter patients with symptoms consistent with Leishmaniasis to ask their patients for a complete travel history to help assess the probability of infection. If infection is suspected, cutaneous Leishmaniasis “can be tested by polymerase chain reaction (PCR) or by doing a culture to identify the type of Leishmania and determine how aggressively it should be treated. A blood test called rK39 provides a rapid result if VL is suspected, which would be confirmed with PCR or culture,” according to the press release. If a patient is determined to be infected, one treatment option is oral miltefosine, which the US Food and Drug Administration (FDA) approved in 2014 to treat some cases of the three main forms of Leishmaniasis. Two alternative options are the ThermoMed device which is used to heat treat cutaneous Leishmaniasis, and another FDA-approved medication, liposomal amphotericin B, which is given intravenously for visceral Leishmaniasis. According to the press release, these treatments are only a little over 80% effective for treating the infection and so “sometimes additional treatment is necessary.” The strongest course of action is to try and avoid the infection in the first place, and so, “wearing protective clothing (long sleeves and pants), applying insect repellents containing DEET, and using insecticide-impregnated bed nets” is best should an individual be traveling to areas of known Leishmaniasis infection.
- See more at: http://www.contagionlive.com/news/deadly-parasitic-disease-finding-its-way-to-us-soil#sthash.w5RlX5g7.dpuf